Westfund collective:

Winners of the Major Grants - Round One 2023, Westfund Community Grants Program
The $40,000 in major grants is in addition to over $100,000 in regular grants and defibrillators awarded by Westfund in this round of the program – our biggest round to date.
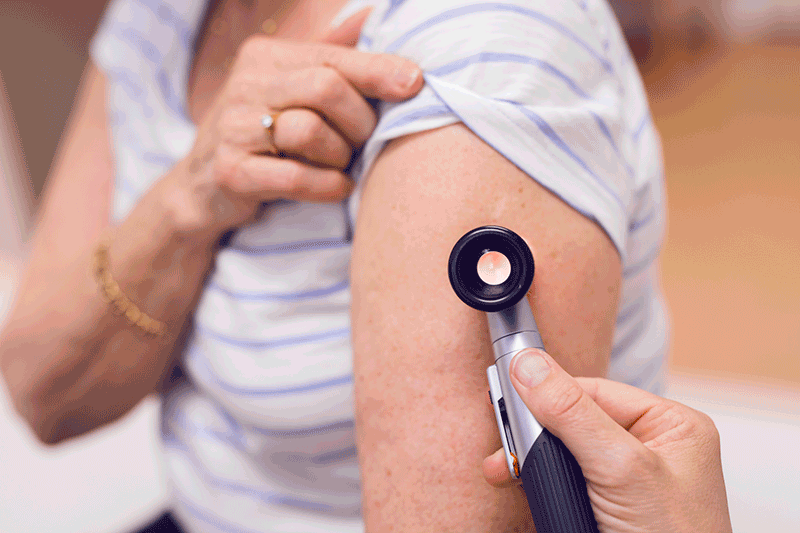
Why are skin checks important?
Having good friends makes you feel good – which has positive effects on your mental wellbeing. Here are some great ways to form connections with other people in your area.

How to connect with your community
Having good friends makes you feel good – which has positive effects on your mental wellbeing. Here are some great ways to form connections with other people in your area.

Looking after yourself, when you’re looking after someone else
When a loved one is struggling, it’s natural that most of your focus will go onto them. But it’s crucial that you don’t stop supporting yourself in the process.

Nervous about using telehealth? Read this
Telehealth might be unfamiliar, but it’s easy to use. Digital health expert Dr Amandeep Hansra shares her advice on getting started.

How to exercise if you don't like exercise
We know that being active is good for physical and mental health, but if you’re not doing enough exercise, the idea of starting can seem all too hard. These tips can help you get moving.